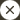The totally different coloured tops of blood assortment tubes point out the presence of particular components. These components serve to both forestall blood clotting or to facilitate the isolation of explicit blood elements. A phlebotomist or different healthcare skilled selects a specific tube coloration primarily based on the diagnostic evaluation requested by a doctor.
Correct choice is vital for correct laboratory outcomes. Utilizing the wrong tube could compromise the pattern, resulting in inaccurate check outcomes and probably impacting affected person care selections. The standardization of color-coding assists healthcare professionals in effectively and reliably amassing the suitable specimens. This methodology reduces the prospect of errors that might consequence within the want for repeat blood attracts, inflicting affected person discomfort and growing healthcare prices. The adoption of this method has considerably improved the accuracy and effectivity of diagnostic testing worldwide.
The next sections will elaborate on the varied tube colours, the components every accommodates, and the sorts of assessments for which every particular tube is meant. This detailed overview offers a sensible information for understanding blood assortment protocols.
1. Components
The components current inside evacuated blood assortment tubes are important elements dictating the kind of evaluation that may be carried out on the collected pattern. Every additive serves a particular goal, interacting with the blood pattern to protect it in a specific state or to facilitate the separation of sure elements. The colour of the tube prime corresponds on to the additive contained inside.
-
Anticoagulants
These substances inhibit the clotting course of, permitting entire blood or plasma to be analyzed. Frequent anticoagulants embrace EDTA (ethylenediaminetetraacetic acid), heparin, and citrate. EDTA, present in lavender-top tubes, chelates calcium ions, stopping coagulation and preserving blood cell morphology for hematology assessments like full blood counts (CBC). Heparin, in green-top tubes, inhibits thrombin formation and is utilized for plasma chemistry assessments. Citrate, in mild blue-top tubes, additionally binds calcium however is reversible, making it appropriate for coagulation research equivalent to prothrombin time (PT) and partial thromboplastin time (PTT).
-
Clot Activators
Conversely, some tubes include substances that promote blood clot formation. These activators, like silica particles or thrombin, speed up the coagulation cascade. Pink-top tubes, typically with out components, depend on the pure clotting course of to yield serum. Serum separator tubes (SSTs), with a gel separator, additionally include clot activators. After centrifugation, the gel types a barrier between the serum and the clot, permitting for straightforward separation and evaluation of the serum part, which is significant for varied chemistry and serology assessments.
-
Preservatives
Sure components act as preservatives, sustaining the soundness of particular analytes inside the blood pattern. For instance, gray-top tubes containing sodium fluoride, an antiglycolytic agent, and potassium oxalate, an anticoagulant, are used for glucose testing. Sodium fluoride inhibits the enzymatic breakdown of glucose, guaranteeing correct glucose degree dedication, significantly when delays in processing are anticipated. These preservatives are important for assessments the place analyte degradation might compromise outcomes.
-
Separator Gels
Many tubes incorporate inert gels that, upon centrifugation, kind a bodily barrier between the mobile elements of blood and the serum or plasma. These gels forestall the re-mixing of cells and fluid, guaranteeing the integrity of the pattern throughout transport and storage. Serum separator tubes (SSTs) and plasma separator tubes (PSTs) exemplify this. The gel in SSTs separates serum, whereas PSTs separate plasma, streamlining laboratory procedures and sustaining pattern high quality for downstream analyses.
The choice of a blood assortment tube with the suitable additive is essential for acquiring correct and dependable laboratory outcomes. The interplay between the additive and the blood pattern dictates the kind of evaluation that may be carried out, and any deviation from the right tube sort can compromise the integrity of the specimen and result in inaccurate diagnostic data. Due to this fact, an intensive understanding of the components current in every tube coloration is important for all healthcare professionals concerned in blood assortment.
2. Shade Standardization
Shade standardization in blood assortment tubes is a vital part of pre-analytical high quality management in laboratory drugs. The established color-coding system straight correlates a particular tube coloration with a delegated additive or lack thereof, thereby indicating the supposed use for explicit laboratory assessments. This standardization reduces the potential for errors in pattern assortment and processing, performing as a visible cue for healthcare professionals to pick out the suitable tube for the required evaluation. Deviation from this established color-coding can result in misguided check outcomes and probably impression affected person care selections. For instance, if a lavender-top tube (EDTA anticoagulant) is mistakenly used as an alternative of a red-top tube (no additive) for a serum chemistry check, the EDTA will intervene with enzymatic reactions, resulting in inaccurate outcomes.
Worldwide organizations, such because the Worldwide Group for Standardization (ISO), have performed a major position in defining and selling coloration standardization in blood assortment. This international standardization permits constant observe throughout totally different healthcare settings and international locations. Standardized colours facilitate the coaching of phlebotomists and laboratory personnel, guaranteeing that each one members of the healthcare group perceive the connection between tube coloration and check necessities. Furthermore, automated laboratory methods depend on coloration recognition to streamline pattern processing, enhancing effectivity and decreasing the chance of human error.
In abstract, coloration standardization in blood assortment tubes is just not merely a matter of comfort however a elementary side of guaranteeing accuracy and reliability in laboratory diagnostics. The adherence to those coloration requirements is important for stopping pre-analytical errors, sustaining pattern integrity, and in the end, supporting optimum affected person care. Whereas challenges could come up in implementing these requirements persistently throughout numerous healthcare environments, the advantages of minimizing errors and bettering effectivity outweigh the difficulties. This understanding of coloration standardization types the bedrock of sound laboratory observe.
3. Check Specificity
Check specificity dictates the kind of blood assortment tube required for correct evaluation. The correlation is direct: the supposed analyte and analytical methodology decide the mandatory components or lack thereof inside the tube. Utilizing the wrong tube compromises the pattern and invalidates the check. For instance, measuring glucose in a serum pattern requires a red-top tube (no additive or clot activator) or a serum separator tube (SST). Using a lavender-top tube, containing EDTA, will bind calcium ions, inhibiting enzymatic reactions needed for glucose measurement, resulting in a falsely low consequence. The specificity of the glucose check necessitates a tube that enables serum separation with out interfering with the analytical course of.
One other instance is in coagulation testing. Prothrombin time (PT) and partial thromboplastin time (PTT) assays, which assess the blood’s clotting capacity, require a light-weight blue-top tube containing sodium citrate. Citrate acts as a reversible anticoagulant, preserving the integrity of clotting elements whereas stopping untimely coagulation. If a special tube, equivalent to a green-top heparin tube, have been used, the check could be invalid because of heparin’s irreversible inhibition of thrombin, altering the clotting profile and rendering the outcomes unreliable. Thus, the precise necessities of coagulation assessments mandate the citrate-containing tube to make sure correct evaluation of clotting perform.
In abstract, check specificity is inextricably linked to blood assortment tube choice. Every diagnostic assay calls for a particular atmosphere inside the assortment tube to make sure correct and dependable outcomes. Incorrect tube choice introduces pre-analytical errors that may result in misdiagnosis and inappropriate therapy selections. Due to this fact, healthcare professionals should perceive the precise necessities of every check and select the corresponding blood assortment tube accordingly. This understanding is vital for sustaining the integrity of laboratory testing and delivering optimum affected person care.
4. Order of Draw
The sequence during which blood assortment tubes are crammed throughout phlebotomy, termed the order of draw, is essential for minimizing the danger of cross-contamination between tube components. Additive carryover can considerably alter laboratory check outcomes, resulting in inaccurate diagnoses and probably dangerous therapy selections. The established order mitigates this danger by guaranteeing that tubes containing essentially the most interfering components are drawn final, minimizing their impression on subsequent samples. As an illustration, if a tube with EDTA is drawn earlier than a coagulation tube, even minute quantities of EDTA carryover can falsely lengthen clotting instances. It is because EDTA chelates calcium, a significant part within the coagulation cascade. Due to this fact, following the right order is just not merely procedural, however a direct safeguard in opposition to analytical error.
The commonly accepted order of draw, primarily based on suggestions from organizations equivalent to CLSI (Medical and Laboratory Requirements Institute), sometimes begins with sterile blood tradition bottles to reduce contamination danger, adopted by non-additive tubes (e.g., red-top tubes for serum), coagulation tubes (e.g., mild blue-top tubes containing citrate), after which tubes with different components equivalent to heparin (green-top), EDTA (lavender-top), and at last, tubes with glucose inhibitors (gray-top). This particular sequence accounts for the potential for additive carryover and the sensitivity of assorted laboratory assessments to those interferences. Failure to stick to this order can result in spurious outcomes, necessitating repeat blood attracts and delaying affected person care. For instance, drawing a heparin tube earlier than a red-top tube might result in heparin contamination, falsely elevating liver enzyme ends in the serum pattern.
In conclusion, the order of draw is an indispensable part of correct blood assortment approach, intricately linked to the right choice of blood assortment tubes for particular assessments. Adherence to the beneficial sequence prevents additive cross-contamination, guaranteeing the accuracy and reliability of laboratory outcomes. Whereas challenges in implementation could come up because of variations in scientific settings or patient-specific elements, the constant utility of the order of draw stays a cornerstone of high quality laboratory observe and optimum affected person care. Recognizing the importance of this relationship promotes a discount in pre-analytical errors, in the end enhancing the utility of diagnostic testing.
5. Pattern Integrity
Pattern integrity is a paramount concern in laboratory diagnostics. It’s inextricably linked to the right choice of blood assortment tubes, because the integrity of a blood pattern straight influences the accuracy and reliability of subsequent check outcomes. Selecting the best tube coloration for a given check is the primary essential step in preserving the pattern’s inherent properties and stopping pre-analytical errors that may compromise diagnostic accuracy.
-
Additive Compatibility
Components inside blood assortment tubes are chosen to both forestall coagulation or protect particular blood elements. Pattern integrity is compromised when incompatible components are used. For instance, utilizing a lavender-top EDTA tube for a coagulation examine invalidates the outcomes as a result of EDTA chelates calcium, disrupting the clotting cascade. Equally, utilizing a clot activator tube (red-top or SST) for an entire blood assay ends in a pattern unsuitable for evaluation. Preserving the pattern in a state suitable with the supposed check is prime to sustaining its integrity.
-
Order of Draw Affect
The sequence during which blood assortment tubes are crammed straight impacts pattern integrity. Drawing tubes within the incorrect order can result in cross-contamination of components, altering check outcomes. Drawing an EDTA tube earlier than a coagulation tube, as an example, can falsely lengthen clotting instances because of EDTA carryover. Adhering to the established order of draw minimizes additive interference, preserving the integrity of every pattern and guaranteeing correct laboratory findings. That is significantly important in circumstances the place small volumes of blood are collected, the place additive carryover has a proportionally bigger impression.
-
Storage and Dealing with Protocols
Correct storage and dealing with procedures are important for sustaining pattern integrity post-collection. Temperature, time to processing, and agitation throughout transport can all affect the pattern’s stability. For instance, extended publicity to room temperature can degrade glucose ranges in samples collected in non-preservative tubes, resulting in falsely low glucose readings. Equally, mishandling samples for full blood counts (CBC) can result in cell lysis, affecting the accuracy of cell counts. Adherence to standardized protocols minimizes these variables and preserves the inherent properties of the blood pattern.
-
Tube Materials and Design
The fabric composition and design of the blood assortment tubes may affect pattern integrity. Sure tube supplies can work together with particular analytes, resulting in inaccurate measurements. As an illustration, some plasticizers in tube partitions can leach into the pattern, interfering with hormone assays. The design of the tube, together with the stopper and inner coating, should guarantee a safe seal to forestall contamination and evaporation. Choosing tubes which might be inert and correctly designed minimizes these dangers and helps the integrity of the blood pattern all through the pre-analytical part.
Sustaining pattern integrity is a multifaceted course of that begins with deciding on the suitable blood assortment tube. Additive compatibility, adherence to the order of draw, correct storage and dealing with, and tube materials composition all contribute to preserving the pattern’s inherent properties. Every of those aspects underscores the vital significance of understanding the connection between check necessities and blood assortment procedures to make sure correct and dependable laboratory outcomes, in the end benefiting affected person care.
6. Laboratory Protocol
Laboratory protocols are standardized procedures that govern all facets of diagnostic testing, together with specimen assortment, dealing with, processing, and evaluation. The correct correlation between blood assortment tube colours and the assessments for which they’re supposed is a elementary component of those protocols. Strict adherence to those pointers is important for sustaining pattern integrity, stopping pre-analytical errors, and guaranteeing the reliability of laboratory outcomes. Deviations from established protocols can result in compromised samples and probably inaccurate diagnoses.
-
Customary Working Procedures (SOPs)
SOPs present detailed directions for every step of the blood assortment and dealing with course of, specifying the right tube coloration for every check and outlining the order of draw. These procedures are essential for coaching personnel and guaranteeing consistency in observe. For instance, a laboratory’s SOP for coagulation testing will explicitly state {that a} mild blue-top tube containing sodium citrate should be used for prothrombin time (PT) and partial thromboplastin time (PTT) assays. Actual-world deviations from SOPs, equivalent to utilizing an incorrect tube, can result in inaccurate clotting instances, probably affecting anticoagulant remedy administration.
-
High quality Management (QC) Measures
QC measures are carried out to watch and validate the accuracy and reliability of laboratory procedures. These measures embrace common checks on tube expiration dates, visible inspections for tube integrity (e.g., cracks or leaks), and adherence to correct storage circumstances. QC protocols additionally tackle the right use of assortment gadgets, guaranteeing that phlebotomists are educated to appropriately determine and use every tube coloration. Failure to stick to QC measures, equivalent to utilizing expired tubes, can compromise pattern integrity and invalidate check outcomes, resulting in delays in prognosis and therapy.
-
Documentation and Traceability
Complete documentation and traceability are integral elements of laboratory protocols. Every step of the method, from pattern assortment to evaluation, should be documented to take care of an audit path. This contains recording the tube coloration used, the date and time of assortment, and the identification of the phlebotomist. Correct documentation permits for the identification of potential errors and facilitates corrective actions. For instance, if a discrepancy is present in a check consequence, the documentation will be reviewed to find out if an incorrect tube was used throughout assortment. With out thorough documentation, it turns into difficult to determine and resolve pre-analytical errors.
-
Coaching and Competency Evaluation
Efficient coaching applications and competency assessments are essential for guaranteeing that laboratory personnel are proficient in blood assortment methods and perceive the importance of tube coloration choice. Coaching ought to cowl the ideas of phlebotomy, the aim of every additive, and the potential penalties of utilizing the wrong tube. Competency assessments confirm that personnel can appropriately determine tube colours and observe the established order of draw. Insufficient coaching can result in errors in tube choice and pattern assortment, leading to compromised pattern integrity and inaccurate check outcomes. Steady schooling and common competency assessments are important for sustaining excessive requirements of observe.
In abstract, laboratory protocols present a framework for guaranteeing the correct and dependable use of blood assortment tubes in diagnostic testing. Via standardized working procedures, high quality management measures, complete documentation, and efficient coaching applications, laboratories can decrease pre-analytical errors and preserve pattern integrity. Adherence to those protocols is important for translating blood assortment tube choice into correct diagnostic data, in the end supporting optimum affected person care. Correct blood assortment tube utilization inside laboratory protocols ensures the era of dependable information, which is used for medical resolution making.
Regularly Requested Questions
The next questions tackle frequent issues concerning the choice and utilization of blood assortment tubes in laboratory diagnostics. The data offered goals to make clear the importance of tube coloration and its impression on check accuracy.
Query 1: What penalties come up from utilizing an incorrect blood assortment tube?
Using an inappropriate blood assortment tube can result in pre-analytical errors that compromise pattern integrity and invalidate check outcomes. Components current in sure tubes could intervene with the analytical processes required for particular assessments, yielding inaccurate information and probably impacting affected person care selections.
Query 2: Why is there a particular order of draw for blood assortment tubes?
The order of draw is designed to reduce the danger of additive carryover between tubes. Drawing tubes within the incorrect sequence can result in contamination, altering check outcomes and compromising the accuracy of diagnostic findings. Adhering to the beneficial order mitigates these potential interferences.
Query 3: How does the additive inside a blood assortment tube have an effect on the check consequence?
Components play a vital position in preserving the blood pattern in a state appropriate for the supposed evaluation. Anticoagulants, clot activators, and preservatives every have particular capabilities that straight affect the accuracy of check outcomes. Utilizing a tube with an incompatible additive can result in inaccurate measurements and compromise pattern integrity.
Query 4: Are there worldwide requirements for blood assortment tube colours?
Whereas some variations exist, worldwide organizations equivalent to ISO promote coloration standardization to make sure consistency throughout totally different healthcare settings. Standardized colours facilitate coaching and decrease the danger of errors in pattern assortment and processing, supporting correct and dependable diagnostic testing worldwide.
Query 5: What’s the significance of a gel separator in sure blood assortment tubes?
Gel separators create a bodily barrier between the mobile elements of blood and the serum or plasma after centrifugation. This barrier prevents the remixing of cells and fluid, guaranteeing the integrity of the pattern throughout transport and storage. This separation is essential for sustaining the soundness of analytes and stopping interference in subsequent analyses.
Query 6: What elements ought to be thought of when deciding on a blood assortment tube for a particular check?
When deciding on a blood assortment tube, the supposed analyte, analytical methodology, additive necessities, and potential interferences should be thought of. Understanding the precise wants of every check and deciding on the suitable tube ensures correct and dependable outcomes, contributing to efficient affected person care.
Correct choice of blood assortment tubes is essential for producing dependable laboratory information, and you will need to seek the advice of laboratory pointers when figuring out the right tube for a specific check. The implications of incorrect tube choice can result in potential misdiagnosis or mistreatment of sufferers.
The following part will delve into assets for additional studying and correct blood assortment protocols.
Suggestions
The next suggestions are essential for correct blood assortment, emphasizing the connection between tube coloration and supposed laboratory evaluation.
Tip 1: Prioritize constant adherence to laboratory customary working procedures (SOPs). These protocols present detailed directions concerning the right tube coloration for every check, minimizing pre-analytical errors.
Tip 2: Emphasize steady coaching for phlebotomists and healthcare personnel. Common coaching periods ought to concentrate on correct blood assortment methods, together with the precise components in every tube and the potential penalties of incorrect tube choice.
Tip 3: Implement stringent high quality management measures. Confirm tube integrity, verify expiration dates, and frequently assess compliance with the established order of draw to forestall pattern contamination and guarantee correct outcomes.
Tip 4: Keep meticulous documentation for all blood assortment procedures. Document the date, time, tube coloration, and phlebotomist identification to create a transparent audit path, facilitating the identification and backbone of potential errors.
Tip 5: Perceive the precise necessities of every laboratory assay. Think about the supposed analyte, analytical methodology, and potential interferences when deciding on a blood assortment tube to make sure that the pattern is collected and preserved in a way suitable with the check.
Tip 6: Acknowledge the significance of correct storage and dealing with. Temperature, time to processing, and agitation throughout transport can all have an effect on pattern stability. Adhere to established protocols to reduce these variables and protect the integrity of the blood pattern.
Tip 7: Seek the advice of laboratory assets and pointers when unsure about blood assortment tube choice. Reference supplies, equivalent to laboratory manuals or on-line databases, present detailed data on the suitable tube coloration for particular assessments.
These pointers guarantee accuracy, scale back the danger of pre-analytical errors, and preserve the integrity of blood samples used for diagnostic testing. Strict adherence to those practices promotes dependable laboratory outcomes and optimum affected person care.
The concluding part will present a abstract and last ideas on the significance of correct blood assortment methods.
Conclusion
The foregoing exploration of “blood tube colours for which check” underscores the vital position of acceptable blood assortment practices in laboratory drugs. The correlation between tube coloration, additive, and supposed evaluation is prime to producing correct and dependable diagnostic data. Adherence to standardized protocols, together with the right order of draw and correct dealing with procedures, minimizes pre-analytical errors and safeguards pattern integrity.
Given the direct impression on affected person care, a dedication to steady schooling and rigorous high quality management in blood assortment is important for all healthcare professionals. Additional analysis and standardization efforts are warranted to optimize blood assortment methods and improve the general accuracy of laboratory diagnostics. This meticulous consideration to element not solely improves the standard of laboratory outcomes but in addition reinforces the dedication to efficient and knowledgeable medical decision-making.